Let’s get it clear: What makes a good cushion?
By Dr Barend ter Haar
Why cushions need to vary from user to user
This article aims to start getting people thinking more about what goes into a cushion that makes it ‘good’ for one person, but not for another. This article sets the scene, whereas the various headings will be teased out in greater detail in future articles.
What makes a good cushion depends on the needs of the individual. These days we have many procurement departments which treat cushions as commodities and, under the misconception that all cushions are the same, look for what is the lowest priced option – unaware that these are prescription items, with different elements that are relevant to any one individual’s needs. This kind of commodity-oriented generalisation is as useless to the individual as saying all white pills must do the same thing since they are all white.
Around reviewing the suitability of a cushion for an individual, the context in which the cushion is to be used needs to be taken into consideration, such as whether it is to be used in a wheelchair, and consequently whether the wheelchair is the right size and conformation. There are various recent publications¹²³ that cover these aspects in varying levels of detail, the most recent of which is the All Wales Best Practice Guidelines⁴.
Over the years what we in the UK currently call Pressure Ulcers have previously been known as Pressure Sores or Decubitus Ulcers. In North America and the Pacific regions, these are now referred to as Pressure Injuries, and as a result, the likes of the North American Pressure Ulcer Advisory Panel (NPUAP) has renamed itself the North American Pressure Injury Advisory Panel (NPIAP). Europe has chosen to stay with ulcers and stay with the EPUAP name as the related body.
When considering which cushion meets the user’s needs, we have three key criteria to consider. The most important for anyone who is sitting still for any length of time is to look after the user’s tissue integrity. The next is positioning: to what extent do the materials in the cushion assist in maintaining a healthy posture. The third is functionality, over and above the provisions of the first two criteria listed: how well does the cushion enable the user to carry out as normal a daily life as possible.
The user needs to be part of the prescription process, since if they are not happy with the prescribed solution, they are unlikely to use it, and risk their health as a result.
For tissue integrity, over the years we have been concerned about pressure, and we have tended to term much of the skin damage that occurs as pressure ulcers. However, for the health of the skin, there are other ‘extrinsic’ factors that may be as, or more, important. These include the microclimate adjacent to the skin, where temperature and moisture come into play – we all know the effect that having our hands in water for an extended period has on our skin. Even more potentially damaging to the skin are the additional effects of friction and shear forces.
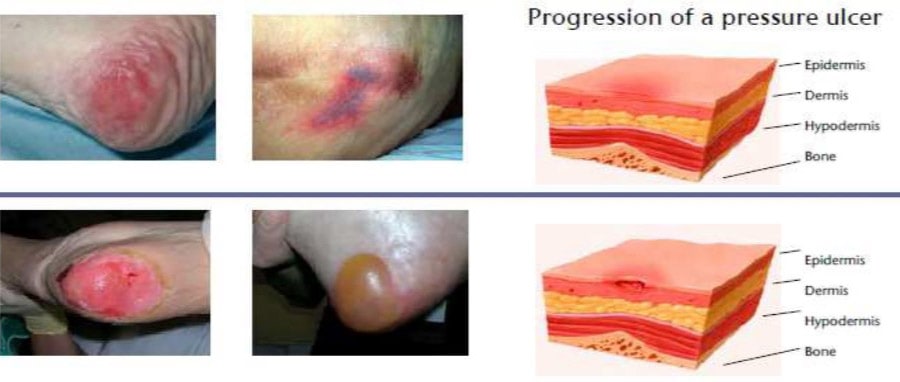
This leads us then not so much to the cushion, as to its cover. The majority of pressure ulcers recorded are Stage 1 or 2, and these occur at the epidermis and dermis, the outer layers of the skin (see Fig. 1).
What affects these outer layers of the skin is what is closest to the skin i.e. one’s clothing and the cover on the cushion. If these items can move with the skin as the person moves in their seat, there will be less risk of shear damage (from shear stress and shear strain) to the skin. Likewise, if the clothing and cover materials control the microclimate from temperature and humidity build-up around the skin, there will be less risk of skin damage arising from a maceration of the skin.
There are over thirty elements, falling under the tissue integrity, postural management, and functionality headings, that can be taken into account when assessing the properties of a cushion and its suitability for an individual. I will be going into these different elements in more detail in future articles.
References
1. BHTA (2018) Get wise to pressure ulcer prevention in sitting: A guide to pressure ulcer prevention in sitting
2. BHTA (2018) Get wise to seated posture: A guide on good seating posture practice
3. Stephens, M & Bartley, C (2018) Understanding the association between pressure ulcers and sitting in adults what does it mean for me and my carers? Seating guidelines for people, carers and health & social care professionals J Tissue Viability 27, 59-73
4. AWTVNE, PUPIS. All Wales Best Practice Guidelines: Seating and Pressure Ulcers. London: Wounds UK, 2019
5. From Pressure Ulcer Prevention and Care for Adults in the Home or Homely Setting NHSTaysidecdn.scot.nhs.uk

Further items can be found at www.beshealthcare.net. If you are interested in receiving further information on the topic, please contact barend@beshealthcare.net.
Dr Barend ter Haar has been involved in seating and mobility for over 30 years, including lecturing internationally and developing international seating standards.