Let’s Get It Clear: Covering a mobility need in a care home
Having been approached a number of times in recent months, by friends and acquaintances in the village in which I live, for advice about equipment to help with their spouses or older relatives, it has become clear that signposting for assistive technology support is desperately needed in the first place, and training in residential and care homes is far from adequate. This ‘Case Study’ highlights these points.
In a small community, what one does in one’s working hours is generally well known. I live in a village with about 120 houses. My neighbour is an esteemed shoulder surgeon at the Royal United Hospital in Bath, and whenever anyone has a shoulder niggle, he’s turned to for advice (shortcutting the GP referral route).
It’s become known that I’ve worked with assistive technology equipment, and so people have been turning to me for advice. In the last nine months, I’ve advised one person about a bath solution for her infirm mother who still wanted to continue to have baths under her own control (and not a shower), and another where he wanted advice for an arm chair for his mobility-impaired wife that could be used in the kitchen while he prepared meals, but compact enough that it could be wheeled into their living room for other times of the day.
The challenge
A third example, and the subject of this case study, relates to another pair of neighbours, in their eighties. A lovely couple, he a tall Scotsman, and she a short Yorkshire lass, have been married 60 years. She had a stroke last autumn affecting one side of her body. She also has quite a degree of senile dementia. He decided, reluctantly, that it would be impractical for her to come home and so she has been in a care home nearby since she left the care of the rehabilitation hospital.
It became clear that she would be spending most of her day in a wheelchair, and because she would be inside most of the time, the local wheelchair service indicated that she did not meet their criteria for provision. What the home had to offer was a basic transit chair on a one size fits all basis, and what her husband wanted was something better fit for purpose. Because he knew I’d been involved with wheelchair equipment for well over 30 years he came to me for advice.
The solution
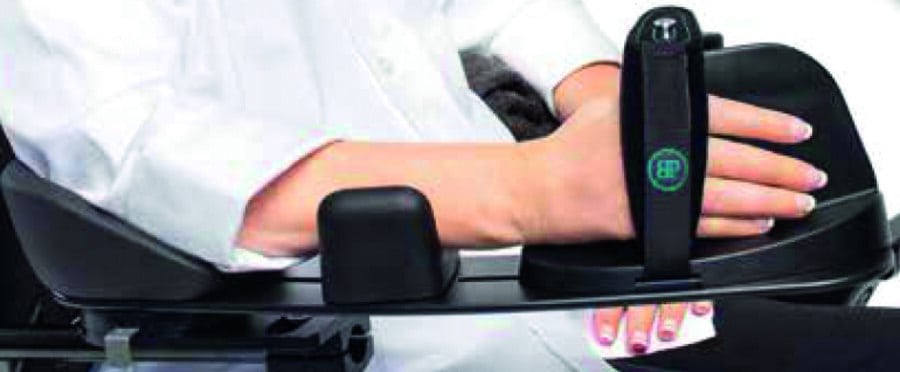
The solution we came up with was a Weely chair with a Varilite Icon Deep back support and Reflex cushion, and a Bodypoint pelvic positioning belt and Bodypoint Dynamic Arm Support dynamic arm support (Figure 1).
The Weely manual chair (Figure 2) with its drive wheels in the midline position is ideal for home use in that this position of the wheels allows for a much smaller turning circle than a conventional manual wheelchair, making it much more manoeuvrable for staff. It also has both recline and tilt facilities, and angle adjustable leg supports, which suited the lady’s changing needs during the day.
A further feature is the ability to lift the front casters over thresholds or kerbs, allowing the chair to go forwards over obstacles, which is more dignified than having to be dragged backwards when outside. The width of the chair was chosen to match Rhoda’s pelvic width, to ensure that she was well supported on either side.
The Reflex cushion was chosen since the air-foam mix would give good skin protection, the internal foam mix gives good positioning support, and the self-setting valve means that it is maintenance free. The newly launched Bodypoint Dynamic Arm Support dynamic arm support was to provide support and movement for the stroke-affected left arm.
What could go wrong?
The care home involved is well run and the staff well-trained in day-to-day care provision. However, early on it became clear that to get the therapeutic benefit of the Bodypoint Dynamic Arm Support (where the user has to be positioned properly in the chair), unfortunately this was not happening frequently enough for the Bodypoint Dynamic Arm Support to be effective, and so it was removed.
The next challenge arose from the behavioural complications of the dementia. The chair user, wanting possibly to feel she had some control of the chair, spent much time putting the brake on and off on one side, and also turning the knob that allowed adjustment of the lower leg support angle. With time this wore away the nut securement part of the knob, and then the knob twirled without resistance.
We have subsequently resolved this by replacing the knob, and then using the ingenuity of our young designer, Peter Horton who used his 3D printer to create a removable cap to go over the knob. The cap could be rotated with enough friction to keep it in place without actually turning the knob (Figure 3 and 4).
When assessing a solution for the knob, we found that despite the chair having been supplied with a specialist cushion to reduce the risk of skin damage, a young nurse had decided to add another, very thick and more basic, cushion on top of the provided cushion (Figure 4). The downside for the user was that she felt much less stable, was positioned badly in a resulting slumped position, and the chair had not been adjusted for the fact that she was now several centimetres higher off the chair’s seat base.
What’s needed?
This case study has raised some important points. The first aspect that needs to be addressed is how the general public can be made better aware of where to turn if they need advice on any and all relevant equipment. In the UK, because the bread and butter end of the business of wheelchair provision, for example, is carried by wheelchair services, this is not passed through dealers, and therefore most UK dealers do not develop the complex breadth and range of product provision that is experienced in other countries.
Also, quite a lot of equipment will come into people’s homes from a loan store, and not from a dealer. The recipient, on the other hand, will only get what the local NHS or social services will offer within their local criteria for support and provision. Many peoples’ needs are therefore not being met by the State, and they are not generally being signposted by the State as to where else to turn.
A knock-on of this is that much equipment that people end up with does not actually meet their needs, in their own homes or in care homes – either because the wrong equipment is being used, or because the carers do not know how to apply the correct equipment to the resident’s needs. This is a worldwide problem.
In Canada, the prevalence of inappropriate wheelchair seating in long term care facilities has been reported to be 58.6%2,3, with common implications being discomfort, poor positioning and mobility, and skin integrity issues. How can we get better training of care home staff as to how to set and use properly the specialist equipment that is supplied to the benefit of the user? Would something simple attached to the equipment with a pictorial guide to the correct set up (the do’s), and parallel guidance for what not to do (the don’ts) make any difference? Ideas welcomed!
References
- ter Haar MB (2023) Managing the upper extremities of the seated person. THIIS July 2023, pp40-42.
- Canada S (2008) Participation and Activity Limitation survey 2006. Ottawa.
- Giesbrecht EM, Mortenson, WB, Miller W (2012) Prevalence and facility level correlates of need for wheelchair seating assessment among long term care residents. Gerontology 58, 378-384.
Further items can be found at www.beshealthcare.net. If you are interested in receiving further information on the topic, please contact 
Dr Barend ter Haar has been involved in seating and mobility for over 30 years, including lecturing internationally and developing international seating standards.




